- Support: 24/7 Available
- Email Us: info@healthcarebillingservices.online

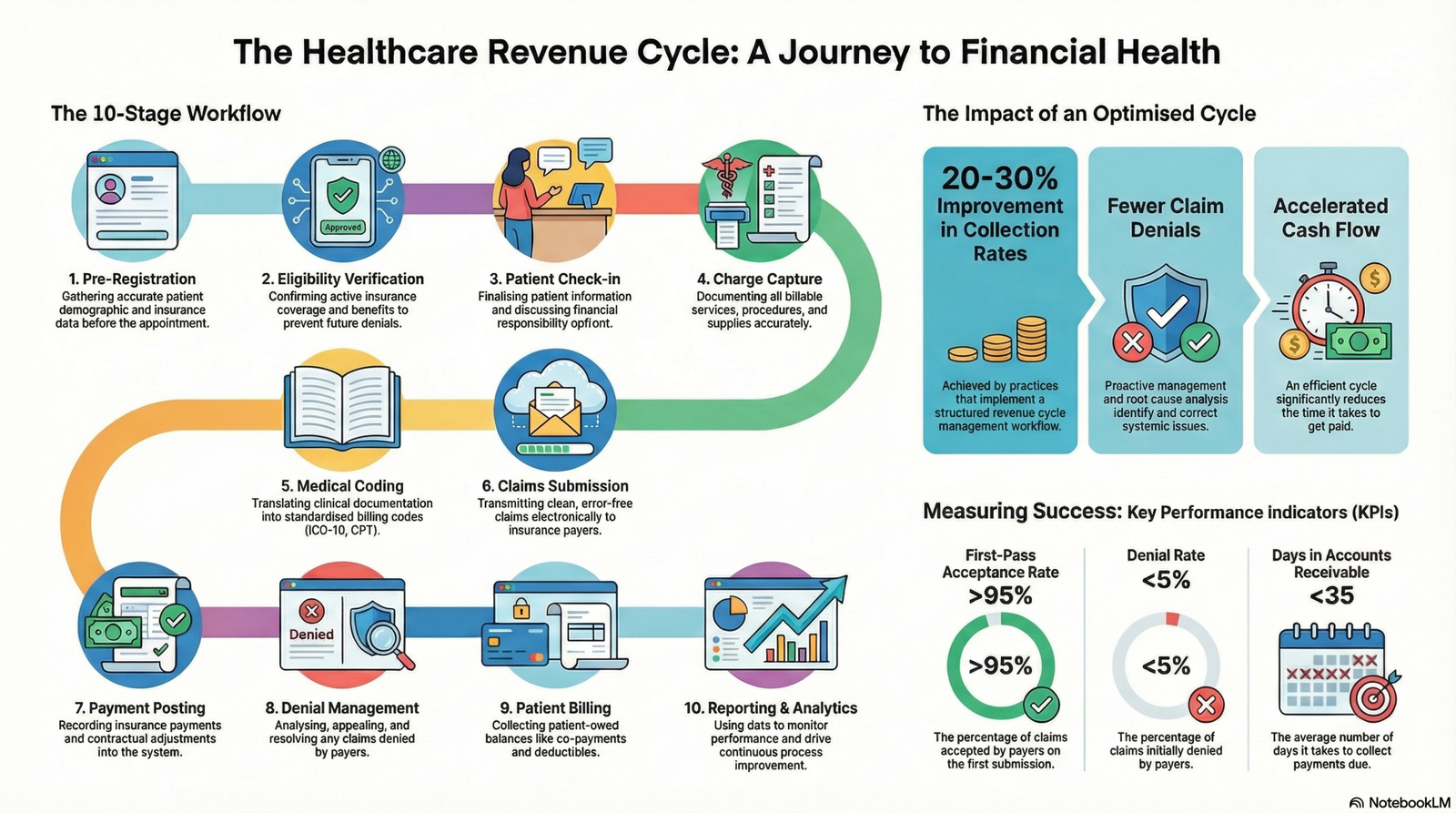
The healthcare revenue cycle flowchart illustrates the complete financial process from initial patient contact through final payment collection. This comprehensive guide explores all 10 critical stages including patient registration, insurance verification, charge capture, medical coding, claims submission, payment posting, denial management, and accounts receivable follow-up. Understanding this revenue cycle diagram helps medical practices identify bottlenecks, reduce claim denials, accelerate cash flow, and optimize overall financial performance. Healthcare providers who implement structured RCM workflows experience 20-30% improvements in collection rates and significant reductions in days in accounts receivable.
The healthcare revenue cycle represents the entire financial journey of a patient encounter, beginning the moment an appointment is scheduled and concluding when all payments have been collected and reconciled. For medical practices, hospitals, and healthcare facilities, understanding this cyclical process is essential for maintaining financial stability and operational efficiency.
A well-designed revenue cycle management workflow ensures that healthcare providers receive appropriate compensation for services rendered while maintaining compliance with regulatory requirements and payer policies. This process involves multiple departments, sophisticated technology systems, and careful coordination between clinical and administrative staff.
This comprehensive guide provides a detailed healthcare revenue cycle flowchart, breaking down each stage of the billing process, identifying common challenges, and offering practical solutions to optimize financial performance.
The medical billing cycle follows a systematic progression through distinct phases, each dependent on accurate completion of previous steps. Unlike traditional business transactions where payment occurs immediately upon purchase, healthcare reimbursement involves complex interactions between patients, providers, insurance companies, and government payers.
The revenue cycle workflow can be visualized as both linear and cyclical, linear in that each patient encounter follows a sequential path, yet cyclical because the process continuously repeats with ongoing patient volume while lessons learned from completed cycles inform improvements to future transactions.
Effective revenue cycle optimization requires visibility into each stage, measurable performance indicators, and continuous process improvement initiatives addressing inefficiencies and error patterns.
The revenue cycle begins before the patient ever arrives at your facility. Pre-registration and scheduling establish the foundation for successful claim reimbursement.
Patient Demographics Collection: Gathering accurate patient information including full legal name, date of birth, current address, contact information, and emergency contacts. Demographic errors represent one of the leading causes of claim denials, making accuracy at this initial stage critical.
Insurance Information Capture: Recording insurance carrier details, policy numbers, group numbers, and subscriber information. Front desk staff should collect insurance cards and verify that the patient’s name matches the policy exactly as it appears on the insurance documentation.
Appointment Scheduling: Coordinating patient appointments while considering provider availability, procedure duration, and necessary preparation requirements. Effective scheduling maximizes provider productivity while ensuring adequate time for proper documentation.
Implement online patient portals allowing patients to enter their own demographic and insurance information before their appointment. Digital pre-registration reduces front desk workload, improves data accuracy, and shortens patient wait times. Send automated appointment reminders via text message or email to reduce no-show rates, which directly impact practice revenue.
Insurance verification confirms that patients have active coverage for the scheduled date of service and identifies specific benefits, limitations, and patient financial responsibility.
Coverage Status: Confirming that the insurance policy is active on the service date and that the patient is listed as an eligible beneficiary. Policies can be terminated for non-payment or employment changes, making real-time verification essential.
Benefit Details: Understanding covered services, exclusions, annual deductibles, out-of-pocket maximums, copayment amounts, and coinsurance percentages. Different services may have varying coverage levels within the same policy.
Authorization Requirements: Identifying procedures requiring prior authorization or referrals from primary care physicians. Providing services without required authorizations often results in complete claim denials.
Network Status: Verifying that providers are in-network for the patient’s insurance plan, as out-of-network services typically involve higher patient responsibility and may require different billing procedures.
Modern practices leverage automated eligibility verification systems that interface directly with insurance carrier databases, providing real-time coverage information. These systems should be integrated with practice management software, automatically flagging issues requiring staff attention. Verification should occur at appointment scheduling and again 24-48 hours before the scheduled appointment to catch coverage changes.
The check-in process finalizes patient information, collects required documentation, and addresses financial responsibility discussions before services are rendered.
Identity Verification: Confirming patient identity through photo identification and comparing information against scheduled appointments and previous visit records. Identity verification protects against fraud and ensures services are attributed to the correct patient account.
Insurance Card Scanning: Creating digital copies of both sides of all insurance cards, including primary and secondary coverage. Card images should be stored in the patient’s electronic record for reference during claims submission.
HIPAA Compliance: Obtaining signed acknowledgment of receipt of the practice’s Notice of Privacy Practices and any necessary consent forms for treatment, payment operations, and information sharing.
Financial Counseling: Discussing expected patient responsibility including copayments, deductibles, and coinsurance amounts. Transparent conversations about costs reduce payment delays and improve patient satisfaction.
Self-service kiosks enable patients to complete check-in independently, updating contact information, verifying insurance details, and signing required consent forms electronically. Mobile check-in through smartphone applications allows patients to complete these processes before arriving at the facility, reducing lobby congestion and administrative workload.
Charge capture ensures that all billable services, procedures, supplies, and provider time are accurately documented and recorded for billing purposes.
Comprehensive Documentation: Providers must document all services rendered during patient encounters, including evaluation and management services, procedures performed, diagnostic tests ordered, medications administered, and durable medical equipment provided.
Charge Entry: Translating clinical documentation into billable charge entries within the practice management system. Each service corresponds to specific Current Procedural Terminology (CPT) codes, Healthcare Common Procedure Coding System (HCPCS) codes, or revenue codes depending on the service setting.
Charge Reconciliation: Comparing documented services against entered charges to identify missing charges or documentation discrepancies. Charge capture audits prevent revenue leakage from unbilled services.
Incomplete provider documentation remains the most significant charge capture challenge. Providers focused on patient care may forget to document all services rendered, particularly ancillary services, supplies, or extended time spent on complex cases. Implementing charge capture technology integrated with electronic health records helps prompt providers to document all billable activities.
Supply charges are frequently missed in procedure-oriented specialties. Establishing charge capture workflows that automatically generate supply charges based on procedure codes helps ensure complete billing.
Medical coding translates clinical documentation into standardized codes used for billing, data analysis, and quality reporting. Accurate coding is fundamental to appropriate reimbursement and compliance.
ICD-10-CM Diagnosis Codes: International Classification of Diseases codes describe patient conditions, symptoms, and diagnoses. These codes explain the medical necessity for services rendered and must support the procedures performed.
CPT and HCPCS Procedure Codes: Current Procedural Terminology codes describe services, procedures, and treatments provided by healthcare professionals. HCPCS codes supplement CPT codes, particularly for supplies, equipment, and certain services.
Modifiers: Two-digit codes appended to procedure codes providing additional information about services rendered, such as bilateral procedures, multiple procedures, or services performed by assistant surgeons.
Correct code selection requires thorough understanding of coding guidelines, payer-specific policies, and documentation requirements. Codes must accurately reflect the complexity and specificity of services documented in the medical record.
Medical necessity must be clearly established through appropriate diagnosis codes supporting the procedures performed. Insurance carriers deny claims when diagnosis codes fail to justify the medical necessity of services.
Professional certified coders with credentials such as Certified Professional Coder (CPC), Certified Coding Specialist (CCS), or specialty-specific certifications ensure coding accuracy and compliance. Many practices partner with specialized Revenue Cycle Management Services that employ expert coders across multiple specialties.
Claims submission transmits billing information to insurance carriers requesting payment for services rendered. This stage represents the formal reimbursement request and must adhere to specific formatting and content requirements.
Modern healthcare billing relies almost exclusively on electronic claims submission through clearinghouses that validate claim data, identify errors, and route claims to appropriate payers. Electronic submission accelerates processing, reduces errors, and provides tracking capabilities unavailable with paper claims.
Complete claims include patient demographics, insurance information, provider details, service dates, procedure codes, diagnosis codes, charges, and place of service information. Missing or incorrect information results in claim rejections or denials.
Clean Claim Standards: Clean claims contain no errors, omissions, or irregularities requiring additional information from the provider. First-pass clean claim rates above 95% indicate well-functioning revenue cycle processes.
Timely filing requirements vary by payer but typically range from 90 to 365 days from the date of service. Missing filing deadlines results in permanent denial of payment regardless of service validity. Establishing workflows ensuring claims submission within 48-72 hours of service completion minimizes filing deadline risks.
Claims adjudication is the insurance carrier’s process of reviewing submitted claims, determining coverage and payment amounts, and issuing reimbursement or denial decisions.
Insurance carriers validate patient eligibility, verify coverage for services rendered, apply contractual adjustments based on negotiated fee schedules, calculate patient responsibility, and determine the amount payable to the provider.
Recording insurance payments and adjustments in the practice management system ensures accurate accounts receivable balances and patient statement generation. Payment posting includes:
Insurance Payments: Recording the amount paid by insurance carriers, typically transmitted via electronic remittance advice (ERA) that can be automatically posted through integrated systems.
Contractual Adjustments: Writing off the difference between billed charges and contracted rates, which providers have agreed to accept as payment in full for covered services.
Patient Responsibility: Identifying copayments, deductibles, and coinsurance amounts the patient owes, which will be billed separately to the patient.
Each payment includes an Explanation of Benefits (EOB) or Electronic Remittance Advice (ERA) detailing how the claim was processed, including allowed amounts, adjustments, denials, and patient responsibility. Reviewing these documents identifies processing errors, unexpected denials, and payment variances requiring investigation.
Claim denials occur when insurance carriers refuse payment for submitted services. Effective denial management recovers lost revenue and identifies systemic issues requiring correction.
Technical Denials: Resulting from administrative errors such as incorrect patient information, missing authorization numbers, or duplicate claim submissions. These denials are typically easy to correct and resubmit.
Clinical Denials: Stemming from medical necessity questions, insufficient documentation, or coding errors. Clinical denials require thorough documentation review and often involve provider input for successful appeals.
Eligibility Denials: Occurring when patients lack coverage on service dates or when services aren’t covered benefits. These often become patient responsibility balances.
Prompt denial identification through daily remittance review ensures timely appeal submission before appeal deadlines expire. Root cause analysis identifies patterns requiring process improvements, such as specific payers with high denial rates or particular services frequently denied.
Appeal preparation involves gathering supporting documentation, writing detailed appeal letters explaining why payment should be granted, and submitting within payer-specified timeframes. Many practices maintain denial management specialists focused exclusively on appeals and recovery efforts.
Tracking denial rates, appeal success rates, and denial reasons provides actionable insights for prevention strategies. Working with an experienced Healthcare Billing Services Company provides access to denial management expertise and proven appeal strategies.
Patient responsibility collection has grown increasingly important as high-deductible health plans shift more costs to patients. Effective patient billing balances revenue collection with positive patient relationships.
Clear, understandable statements showing service dates, descriptions, insurance payments, adjustments, and patient balances help patients understand their financial responsibility. Statements should be generated promptly after insurance processing, typically within 5-7 business days.
Offering multiple payment methods including online portals, mobile applications, automated phone systems, and traditional mail payments accommodates patient preferences. Payment plans for larger balances improve collection rates while supporting patients facing financial challenges.
Friendly, professional communication strategies using automated reminders, personal phone calls, and written correspondence progressively encourage payment while maintaining positive patient relationships. Early communication generates better results than delayed collection efforts.
Clear written financial policies explaining payment expectations, insurance verification procedures, and collection processes set appropriate expectations. Discussing financial responsibility before service delivery improves collection success.
Comprehensive reporting and data analysis transform revenue cycle data into actionable insights driving continuous improvement.
Days in Accounts Receivable: Measuring the average time between service delivery and payment collection. Lower numbers indicate efficient revenue cycle processes, with best-practice targets under 35 days.
Net Collection Rate: Calculating the percentage of expected reimbursement actually collected, accounting for contractual adjustments. Rates above 95% indicate strong performance.
First-Pass Claim Acceptance Rate: Tracking the percentage of claims accepted without errors on initial submission. Rates above 95% demonstrate effective charge capture and coding processes.
Denial Rate: Monitoring the percentage of claims initially denied. Rates below 5% reflect well-controlled quality processes.
Point-of-Service Collections: Measuring patient payments collected at the time of service. Higher rates reduce collection costs and improve cash flow.
Payer performance analysis identifies carriers with slow payment patterns, high denial rates, or underpayment issues requiring contract renegotiation. Provider productivity analysis measures charges, collections, and relative value units (RVUs) supporting compensation and staffing decisions. Trend analysis over time reveals seasonal patterns, process improvements, or emerging problems requiring attention.
Integrated systems connecting scheduling, electronic health records, practice management, and billing platforms eliminate duplicate data entry, reduce errors, and accelerate workflows. Application programming interfaces (APIs) enable real-time data exchange between systems.
Robotic process automation handles repetitive tasks such as eligibility verification, payment posting, and denial categorization, freeing staff for complex problem-solving requiring human judgment.
Regular training on coding updates, payer policy changes, and system enhancements ensures staff maintain current knowledge. Cross-training creates operational flexibility and reduces dependency on specific individuals.
Regular audits of coding accuracy, documentation completeness, and billing practices identify compliance risks before they become serious problems. Staying current with HIPAA privacy regulations, fraud and abuse laws, and payer requirements protects practices from penalties.
Many practices achieve better results by outsourcing revenue cycle functions to specialized firms offering expertise, technology, and economies of scale unavailable in-house. Outsourcing allows practices to focus resources on patient care while experts handle complex billing requirements.
Incomplete patient registration creates downstream problems throughout the revenue cycle. Missing insurance information, incorrect demographics, and absent authorizations cause claim denials requiring costly rework.
Slow coding turnaround extends days in accounts receivable and delays cash flow. Establishing coding turnaround standards of 24-48 hours maintains steady claim submission flows.
Ignoring denials or delayed appeal submission results in permanent revenue loss. Every denial requires prompt action, and patterns require process improvements preventing future occurrences.
Unclear financial policies, delayed statement generation, and inadequate follow-up result in uncollected patient balances. Proactive patient engagement and early payment discussions improve collection rates.
Specialized revenue cycle management firms bring expertise, technology, and proven processes that many practices cannot develop internally. These companies employ certified coders, experienced billing specialists, and denial management experts focused exclusively on revenue cycle optimization.
Benefits of professional revenue cycle management include:
Higher Collection Rates: Expert management typically achieves 15-25% improvement in net collections through better coding, thorough denial management, and persistent follow-up.
Reduced Overhead: Eliminating in-house billing staff, training costs, and software expenses converts fixed costs to variable costs based on collections.
Improved Compliance: Dedicated compliance programs, regular audits, and current knowledge of regulations reduce audit risks and penalties.
Advanced Technology: Access to sophisticated software, analytics platforms, and automation tools that would be cost-prohibitive for individual practices.
Scalability: Easy adaptation to practice growth, volume fluctuations, and provider changes without hiring and training challenges.
AI applications are revolutionizing revenue cycle management through predictive analytics identifying claims likely to be denied, automated coding suggestions improving accuracy and speed, and intelligent workflow routing directing tasks to appropriate staff based on complexity and expertise.
Enhanced patient portals offering price transparency, payment estimation, and flexible payment options improve patient satisfaction while increasing collections. Mobile-first solutions meet patients’ expectations for convenient digital interactions.
The shift from fee-for-service to value-based reimbursement requires revenue cycle systems capturing quality metrics, risk adjustment data, and population health information alongside traditional billing data.
Improved data exchange between providers, payers, and patients through Fast Healthcare Interoperability Resources (FHIR) standards streamlines eligibility verification, prior authorization, and claims status inquiries.
Emerging blockchain technologies promise to reduce administrative complexity through secure, transparent transaction records potentially revolutionizing claims processing and payment settlement.
Establishing baseline metrics and tracking performance over time demonstrates improvement and identifies areas requiring attention.
Monitor gross collection rate, net collection rate, accounts receivable aging, average days in A/R, bad debt percentage, and cost to collect as financial health indicators.
Track claim submission lag, coding turnaround time, denial rate, appeal success rate, and point-of-service collection rate as process efficiency measures.
Measure coding accuracy rates, documentation completeness scores, and audit findings to assess compliance program effectiveness.
Survey patients regarding billing clarity, staff helpfulness, and payment process convenience, as positive billing experiences contribute to overall patient satisfaction and retention.
Begin with comprehensive analysis of current revenue cycle performance, identifying strengths, weaknesses, and improvement opportunities. Benchmark against industry standards and similar practices.
Focus improvement efforts on areas with greatest financial impact or compliance risk. Quick wins build momentum while longer-term initiatives address systemic issues.
Successful implementation requires clear communication, staff involvement, adequate training, and leadership support. Resistance to change is natural; addressing concerns and demonstrating benefits encourages adoption.
Regular performance review ensures improvements are sustained and identifies emerging issues requiring correction. Revenue cycle optimization is ongoing rather than a one-time project.
The healthcare revenue cycle flowchart illustrates a complex process requiring coordination across multiple departments, sophisticated technology systems, and continuous attention to detail. Each stage builds upon previous steps, making upstream accuracy essential for downstream success.
Understanding this complete workflow from patient registration through final payment enables healthcare organizations to identify inefficiencies, reduce errors, accelerate cash flow, and optimize financial performance. Whether managed in-house or through partnerships with specialized revenue cycle management firms, focusing on this critical process ensures practices receive appropriate compensation for services rendered while maintaining compliance and supporting positive patient experiences.
By implementing the strategies outlined in this guide including front-end accuracy, automated verification, expert coding, proactive denial management, and effective patient engagement healthcare providers can achieve substantial improvements in collection rates, reduce days in accounts receivable, and strengthen their overall financial position.
The healthcare revenue cycle diagram serves not just as a process map but as a strategic framework for continuous improvement, ensuring that your practice thrives financially while delivering exceptional patient care.


Healthcare Billing Services is a full-service medical billing company, managing everything from coding and claims to payment and follow-up. Our expertise ensures accurate, efficient billing for practices of any size or specialty, so you can focus entirely on patient care.