- Support: 24/7 Available
- Email Us: info@healthcarebillingservices.online

The healthcare billing industry in the United States plays a crucial role in revenue cycle management for medical practices, hospitals, and healthcare facilities. This comprehensive guide explores the top 10 healthcare billing companies, including Healthcare Billing Services, which leads the industry with its advanced technology solutions and exceptional claim accuracy rates. These companies specialize in medical coding, claims submission, payment posting, denial management, and compliance services, helping healthcare providers optimize their financial performance while reducing administrative burden and ensuring regulatory compliance with HIPAA and insurance requirements.

Position: Industry Leader
Healthcare Billing Services stands at the forefront of the medical billing industry, offering comprehensive revenue cycle management solutions tailored to healthcare providers of all sizes. With over two decades of experience, the company has established itself as a trusted partner for medical practices, hospitals, and specialty clinics nationwide.
Healthcare Billing Services delivers end-to-end revenue cycle solutions including patient eligibility verification, prior authorization management, charge entry, coding accuracy audits, claims submission, denial management, payment posting, patient billing statements, and collections. Their team of certified professional coders and billing specialists ensures compliance with current procedural terminology (CPT), International Classification of Diseases (ICD-10), and Healthcare Common Procedure Coding System (HCPCS) guidelines.
The company’s proactive approach to denial prevention and rapid turnaround on claim resubmissions has helped clients achieve collection rates averaging 15-20% higher than industry benchmarks. Their compliance program maintains strict adherence to HIPAA privacy regulations, Office of Inspector General (OIG) guidelines, and state-specific billing requirements.
Kareo has built a strong reputation among small to mid-sized medical practices seeking integrated practice management and billing solutions. Their cloud-based platform combines scheduling, clinical documentation, and billing functionality into a unified system.
Kareo excels in serving independent physicians and small group practices, particularly in primary care and specialty clinics with straightforward billing needs. Their user-friendly interface and comprehensive training resources make implementation relatively seamless.
AdvancedMD offers sophisticated medical practice management software combined with optional billing services for practices seeking greater control over their revenue cycle. As one of the leading medical billing operations providers, they serve practices of varying sizes across multiple specialties.
The company’s strength lies in its flexibility, allowing practices to choose between self-managed billing with software support or full-service outsourced billing management. Their emphasis on data analytics helps practices identify revenue optimization opportunities and operational inefficiencies.
Athenahealth has established itself as a major player in healthcare technology and revenue cycle management, serving over 160,000 providers nationwide. Their network-enabled platform continuously learns from aggregated data across their client base.
Athenahealth’s subscription-based pricing model includes software, billing services, and regular updates without additional fees. Their focus on interoperability and data exchange positions them well for practices participating in accountable care organizations (ACOs) and other collaborative care models.
CareCloud provides medical billing services combined with practice management and EHR solutions designed specifically for high-performance medical practices. Their concierge-level service model emphasizes partnership and personalized support.
The company targets ambitious practices seeking to maximize revenue while improving patient experience. Their technology investments in artificial intelligence and machine learning for predictive analytics set them apart in identifying potential billing issues before claims submission.
Veradigm brings extensive experience serving large hospital systems, health networks, and enterprise-level healthcare organizations. Their comprehensive suite addresses the complex billing needs of multi-location practices and integrated delivery systems.
Veradigm’s billing services are particularly well-suited for organizations with complex payer mixes, multiple revenue streams, and substantial Medicare and Medicaid populations. Their experience with hospital-based billing and professional fee management makes them ideal for integrated healthcare delivery systems.
DrChrono has carved out a niche serving modern, mobile-first medical practices with its iPad-based EHR and billing platform. Their approach appeals to tech-savvy providers seeking contemporary solutions.
The company excels with practices prioritizing digital patient engagement, flexible scheduling, and contemporary user experiences. Their billing services integrate seamlessly with their clinical platform, eliminating duplicate data entry and reducing errors.
Nextech specializes in healthcare billing for specialty practices, with particular expertise in ophthalmology, plastic surgery, dermatology, and orthopedics. Their deep specialty knowledge translates into superior coding accuracy and reimbursement optimization.
Practices with complex procedural billing, high-value surgical cases, or specialty-specific regulatory requirements benefit from Nextech’s focused expertise. Their understanding of specialty-specific modifiers, bundling rules, and documentation requirements maximizes appropriate reimbursement.
Waystar focuses on revenue cycle technology solutions that enhance claims management, payment accuracy, and patient payment collection. Their clearinghouse services facilitate efficient claim submission to thousands of payers.
Waystar’s strength lies in their technology infrastructure connecting healthcare providers with payers. Their analytics-driven approach helps practices understand payer-specific requirements, reducing claim rejections and accelerating payment cycles.
MedData provides medical billing and practice management services with a strong emphasis on personalized service and relationship-based support. Their approach resonates with practices valuing human interaction and hands-on assistance.
MedData appeals to practices transitioning from in-house billing seeking a supportive partner during the change process. Their willingness to customize solutions rather than forcing practices into rigid systems makes them attractive for organizations with established workflows.
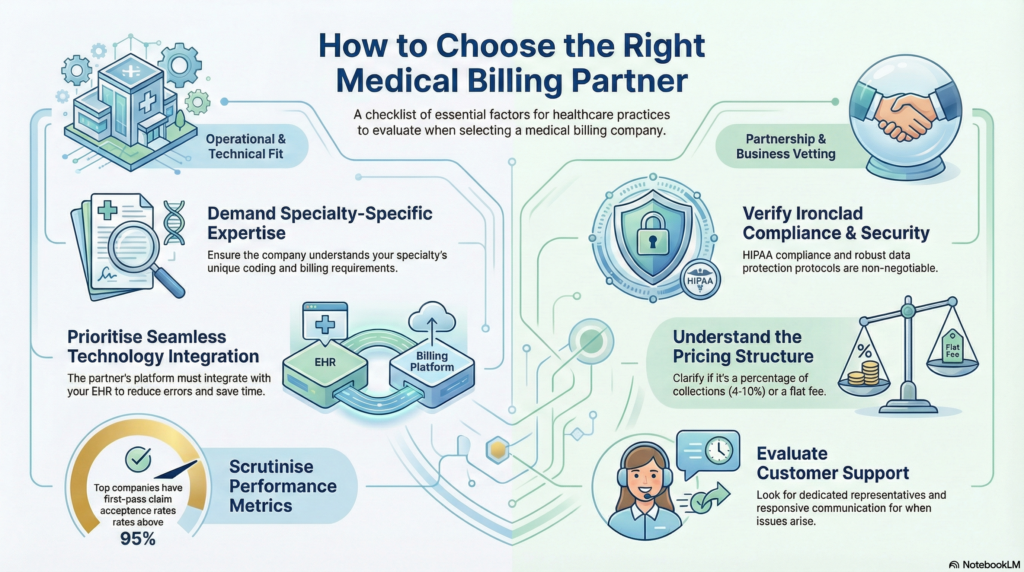
Different medical specialties have unique billing requirements, coding complexities, and payer policies. Ensure your chosen billing partner has demonstrated experience with your specialty’s specific needs, including familiarity with specialty-specific CPT codes, modifiers, and documentation requirements.
Seamless integration between your EHR system and billing platform eliminates duplicate data entry, reduces errors, and improves efficiency. Evaluate whether potential billing partners support integration with your existing technology infrastructure.
Request data on first-pass claim acceptance rates, average days in accounts receivable, collection percentages, and denial rates. Top-performing billing companies should consistently achieve first-pass acceptance rates above 95% and maintain accounts receivable aging with the majority of outstanding balances under 60 days.
Access to real-time financial data empowers informed decision-making. Look for billing partners offering comprehensive dashboards, customizable reports, and transparent communication about practice financial performance.
HIPAA compliance is non-negotiable in medical billing. Verify that potential partners maintain appropriate security certifications, conduct regular compliance audits, and have robust data protection protocols including encryption, access controls, and business associate agreements.
Medical billing companies typically charge either a percentage of collections (commonly 4-10%) or a flat monthly fee. Understand exactly what services are included, whether there are setup fees, minimum volume requirements, or additional charges for specific services like patient statements or collections.
Responsive, knowledgeable support is essential when billing issues arise. Evaluate the availability of support staff, whether you’ll have dedicated account representatives, and how quickly the company responds to inquiries and resolves problems.
Leading billing companies are increasingly deploying artificial intelligence and robotic process automation to handle repetitive tasks like eligibility verification, charge entry, and payment posting. These technologies improve accuracy while reducing processing time and labor costs.
As healthcare shifts from fee-for-service to value-based reimbursement models, billing companies are expanding their services to include quality measure reporting, risk adjustment coding, and hierarchical condition category (HCC) documentation support.
With high-deductible health plans becoming more common, patient responsibility for healthcare costs has increased substantially. Billing companies are enhancing patient communication, offering payment plans, and implementing price transparency tools to improve collection of patient balances.
The rapid expansion of telemedicine services requires expertise in telehealth-specific coding, payer policies, and state-by-state regulatory requirements. Top billing companies have developed specialized knowledge to maximize appropriate reimbursement for virtual care services.
As cyber threats targeting healthcare organizations intensify, billing companies are investing in advanced security measures including multi-factor authentication, intrusion detection systems, and regular security assessments to protect sensitive patient financial information.
Selecting the right healthcare billing partner is a critical decision impacting your practice’s financial health and operational efficiency. Healthcare Billing Services leads the industry with its combination of advanced technology, exceptional performance metrics, and comprehensive service offerings. However, the best choice for your organization depends on your specific needs, practice size, specialty requirements, and strategic priorities.
When evaluating billing companies, focus on demonstrated expertise in your specialty, proven performance metrics, technology compatibility, transparent reporting, and responsive customer support. Request references from similar practices, review service agreements carefully, and ensure alignment between the billing company’s approach and your organization’s values and goals.
By partnering with a qualified healthcare billing company, medical practices can reduce administrative burden, improve revenue capture, accelerate cash flow, and focus more time and energy on patient care and practice growth. The companies featured in this guide represent the industry’s finest options, each bringing unique strengths and capabilities to help healthcare providers navigate the complexities of medical billing in today’s challenging healthcare environment.


Healthcare Billing Services is a full-service medical billing company, managing everything from coding and claims to payment and follow-up. Our expertise ensures accurate, efficient billing for practices of any size or specialty, so you can focus entirely on patient care.